Varicose veins, a common vascular condition, are often associated with visible symptoms and physical discomfort. While many perceive them as a cosmetic concern, varicose veins can lead to significant pain, impacting the quality of life. Understanding the causes, symptoms, and effective management strategies for varicose vein pain is crucial. This comprehensive guide will explore all aspects of varicose veins pain, offering insights from Dr Sumit Kapadia, a renowned vascular specialist and Varicose veins specialist in Vadodara practising at Aadicura Superspeciality Hospital. His expertise in treating varicose veins provides invaluable guidance for those seeking relief.
Let’s understand who gets Varicose Veins.
Varicose veins are a common vascular condition that can affect a broad range of individuals, but certain groups are more predisposed to developing them. Understanding who is most at risk can help in early identification and management. The major risk factors include:
Genetic Predisposition: One of the primary risk factors for varicose veins is heredity. If other family members have varicose veins, the likelihood of developing them increases significantly.
Gender and Hormonal Factors: Women are more likely to develop varicose veins compared to men. This disparity is partly due to hormonal factors, especially those that occur during pregnancy, menstruation, and menopause. Hormones like progesterone can relax vein walls, leading to varicosities.
Age: As people age, the wear and tear on the vein valves that regulate blood flow increase. Over time, this can weaken the valves and lead to varicose veins. The natural loss of skin elasticity and muscle tone with age also contributes to the development of varicose veins.
Lifestyle and Occupational Factors: Individuals with sedentary lifestyles or those whose occupations require prolonged standing are at higher risk. Sitting or standing for extended periods can increase the pressure in leg veins, exacerbating the risk of varicose veins.
Obesity: Excessive body weight puts additional pressure on the veins, particularly those in the legs. This increased pressure can strain the valves in the veins, leading to varicose veins.
Pregnancy: Pregnancy significantly increases the risk of varicose veins. During pregnancy, the volume of blood in the body increases to support the growing fetus, adding pressure to the veins. Moreover, hormonal changes during pregnancy can also lead to the relaxation of blood vessel walls.
Understanding these risk factors is essential for early intervention and effective management of varicose veins. Individuals who identify with one or more of these risk factors should be vigilant about the health of their veins and seek guidance from varicose veins specialists in Gujarat like Dr Sumit Kapadia.
What are the symptoms of Varicose Veins
Varicose veins, characterized by their enlarged and twisted appearance, manifest a variety of symptoms that can range from mild discomfort to severe pain, affecting daily activities and overall quality of life. Understanding these symptoms is key to recognizing the condition and seeking timely medical intervention.
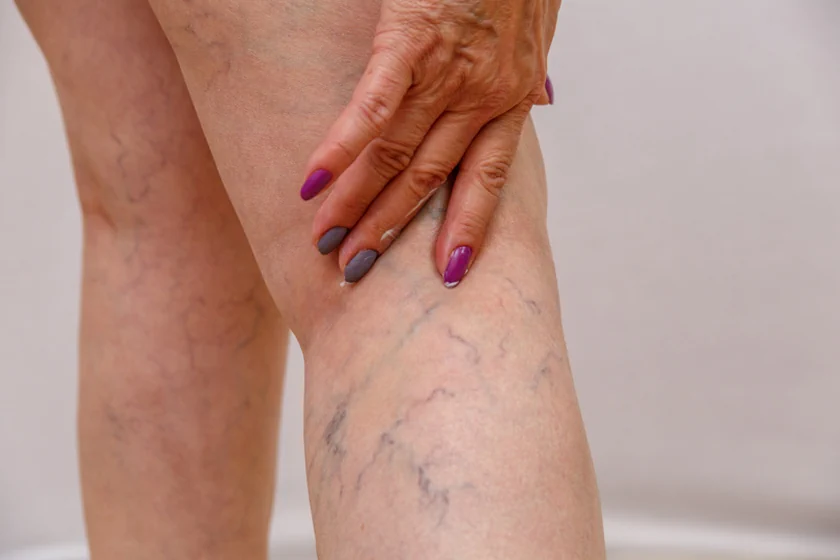
Visible Enlargement of Veins: One of the most noticeable symptoms of varicose veins is the appearance of dark blue or purple veins that are prominently visible beneath the skin surface. These veins often appear swollen, twisted, and bulging, typically on the legs.
Aching Pain: Individuals with varicose veins frequently experience an aching or heavy feeling in their legs. This discomfort is often more pronounced after prolonged periods of standing or sitting and can be a persistent source of discomfort. It is important to note that severe pain especially with difficulty in standing or walking is unlikely to be due to varicose veins. Always consult a doctor to rule out other causes of pain.
Throbbing and Cramping: Varicose veins can cause throbbing sensations or muscle cramping in the legs. These symptoms may worsen at night or after physical activity.
Itching Around Veins: Itching around the affected veins is a common symptom. This itching isn’t just superficial but is often due to the increased pressure within the veins.
Swelling in Lower Legs: Swelling in the feet and ankles is a frequent symptom associated with varicose veins. This swelling is caused by the accumulation of blood in the affected veins, leading to fluid leakage into the surrounding tissues.
Changes in Skin Color and Texture: In advanced cases, there may be changes in skin color around the affected veins, typically leading to a brownish or blueish discolouration. The skin may also become thinner and more fragile over the varicose veins.
Leg Ulcers: In severe cases, particularly when left untreated, varicose veins can lead to the development of ulcers on the skin near the affected veins, particularly near the ankles. Leg ulcers are a serious complication and require immediate medical attention.
It’s important to note that while these symptoms can cause significant discomfort, they are often treatable, especially with early intervention. Dr Sumit Kapadia, a skilled varicose veins surgeon practising at Aadicura Superspeciality Hospital, emphasizes the importance of early diagnosis and treatment. Those experiencing these symptoms should seek professional advice. Timely treatment can alleviate discomfort, prevent complications, and improve overall vein health. To learn more about when to seek medical attention for varicose veins, you can visit Dr. Sumit Kapadia’s blog on varicose vein symptoms.
Why Do Varicose Veins Cause Pain?
Understanding the cause of pain in varicose veins is crucial for effective management and treatment. Varicose veins develop when the valves in the veins, which help regulate blood flow, become weak or damaged. This leads to several physiological changes and symptoms, including pain.
Venous Pressure and Blood Pooling: In healthy veins, valves ensure that blood flows towards the heart. When these valves malfunction, blood can flow backwards and pool in the veins, particularly in the lower legs. This pooling increases the pressure inside the veins, causing them to become enlarged and twisted – the hallmark appearance of varicose veins. The increased pressure and stretching of the vein walls contribute to the pain and discomfort associated with varicose veins.
Inflammation: The accumulation of blood in the veins can lead to inflammation in the vein walls. This inflammation can cause a dull ache or a feeling of heaviness in the legs, often worsened by prolonged standing or sitting. The inflamed veins can also become tender to the touch, making physical activities uncomfortable.
Leg Swelling: The increased pressure in varicose veins often leads to fluid leakage into the surrounding tissues, causing swelling (edema) in the legs and ankles. This swelling can exacerbate the feeling of heaviness, aching, and pain in the legs.
Skin Changes and Ulcers: In advanced cases, the chronic increase in venous pressure can lead to changes in the skin around the varicose veins, including discoloration, dryness, and eczema. In severe cases, it can lead to the formation of ulcers, which can be painful and difficult to heal.
Secondary Conditions: Varicose veins can also lead to the development of other conditions like superficial thrombophlebitis, where a blood clot forms in a vein just below the skin’s surface, causing localized redness, pain, and swelling.
How to manage Varicose Veins Pain?
Effectively managing the pain associated with varicose veins is vital for maintaining quality of life and preventing further complications. Here are several strategies, including lifestyle changes and medical treatments, that can alleviate the discomfort caused by varicose veins:
Elevate Your Legs: Elevating the legs above the heart level several times a day can significantly reduce the pressure in leg veins, helping to alleviate swelling and pain. This simple action encourages blood to flow back towards the heart, reducing the stress on the vein valves and walls. It’s particularly beneficial to elevate your legs for a short period after spending a long time standing or sitting.
Exercise and Stretch Your Legs: Regular physical activity, especially exercises that involve the legs, can improve blood circulation and strengthen the muscles that support your veins. Walking, cycling, swimming, and yoga are excellent choices. These activities help pump the blood back to the heart and can reduce the pressure build-up in the veins.
Use Cold Water: Applying cold water or ice compresses to the affected area can provide immediate, albeit temporary, relief from pain and swelling. The cold helps to constrict the blood vessels, reducing inflammation and discomfort. It’s important to avoid direct contact with extreme cold, so always use a cloth or towel between the ice pack and your skin.
Compression Stockings: One of the most recommended treatments for varicose veins pain management is wearing compression stockings. These stockings apply gradual pressure to the legs, improving venous return and reducing pain and swelling. Dr. Sumit Kapadia often advises patients on the appropriate type and fit of compression stockings, ensuring they are both effective and comfortable.
Pain Medication: Over-the-counter pain relief medications, such as ibuprofen or acetaminophen, can be used to manage mild to moderate pain associated with varicose veins. In cases of more severe pain, it’s important to consult a healthcare professional for suitable prescription medications.
Diet and Hydration: A healthy diet rich in fibre can prevent constipation, which in turn can help reduce the pressure on leg veins. Staying well-hydrated also helps maintain good circulation and vein health.
Professional Treatment: For persistent varicose vein pain, seeking treatment from a varicose veins specialist like Dr. Sumit Kapadia is very important. Treatments can range from minimally invasive procedures like sclerotherapy and endovenous laser therapy to more traditional surgical options, depending on the severity of the condition.
How to Prevent Varicose Veins
Preventing varicose veins, particularly for those at higher risk, involves proactive measures that focus on improving blood circulation and strengthening vein walls. Here are several effective strategies:
Regular Physical Activity: Engaging in regular exercise is one of the most beneficial ways to prevent varicose veins. Activities like walking, swimming, cycling, and yoga improve circulation in the legs and strengthen the muscles that support the veins. These exercises facilitate the upward flow of blood back to the heart, reducing the pressure on leg veins.
Maintaining a Healthy Weight: Excess body weight can put additional pressure on the veins, particularly in the lower body. By maintaining a healthy weight through a balanced diet and regular exercise, one can reduce this pressure and lower the risk of developing varicose veins.
Proper Leg Elevation: Elevating the legs above the level of the heart, especially after standing for long periods, can help blood flow back to the heart and relieve pressure on the veins. This can be done by lying down and resting the legs on a pillow or an elevated surface.
Compression Stockings: Compression stockings are specially designed to apply gentle pressure to the legs, promoting blood flow and reducing the risk of blood pooling in the veins. They are particularly beneficial for individuals who are prone to varicose veins or spend a lot of time standing. Dr Sumit Kapadia often recommends the use of compression stockings as a preventive measure, especially for those with a family history of varicose veins or during pregnancy. Here’s a useful video on the benefits of compression stockings.
Avoid Prolonged Standing or Sitting: Standing or sitting for extended periods can increase the pressure in the veins and hinder blood flow. It’s important to take regular breaks to move around or change positions to improve circulation.
Healthy Diet: A diet rich in high-fibre foods can prevent constipation, which can put additional pressure on the veins. Including foods high in flavonoids, such as vegetables and berries, can also help improve blood circulation and keep the veins strong.
Proper Footwear and Clothing: Wearing comfortable, low-heeled shoes and avoiding tight clothing around the waist and thighs can improve blood flow and reduce the risk of varicose veins.
When to See a Doctor for varicose veins pain
Recognizing when to seek medical attention for varicose veins is crucial in preventing complications and ensuring effective treatment. Varicose veins not only cause discomfort but can also lead to more serious health issues if left unaddressed. Here are key indicators that it’s time to consult a doctor, particularly a varicose veins surgeon like Dr. Sumit Kapadia:
- Persistent Pain and Discomfort
- Severe Swelling
- Formation of Ulcers
- Blood Clots or Bleeding
- Lifestyle Limitations
- Ineffectiveness of Home Remedies
To effectively manage the pain associated with varicose veins, it is essential to address both the symptoms and the underlying venous insufficiency. Treatment options range from lifestyle modifications, such as regular exercise and leg elevation, to medical interventions like compression therapy and surgery.
Mrs Patel’s Journey Through Varicose Vein Pain to Relief
Once an active school teacher in Vadodara, Mrs. Patel’s (Name changed) life took a challenging turn when she started experiencing leg pain and visible, bulging veins – the classic signs of varicose veins. Initially dismissing it as a mere cosmetic issue, she soon found her daily activities hindered by aching, swelling, and a constant sense of heaviness in her legs. Standing for long hours in the classroom became increasingly difficult, and her walks, which she used to enjoy, turned into a painful ordeal.
The Turning Point:
It was during a family gathering when her niece, a nursing student, noticed the condition of Mrs Patel’s legs and expressed concern. She spoke about the potential risks of untreated varicose veins, including blood clots and ulcers. This conversation was a wake-up call for Mrs Patel, prompting her to seek medical advice.
Consulting with Dr. Sumit Kapadia:
Mrs. Patel scheduled an appointment with Dr. Sumit Kapadia at Aadicura Superspeciality Hospital. Dr. Kapadia, known for his expertise in vascular health, conducted a thorough examination and diagnosed her with advanced varicose veins. He explained how her condition was more than just a cosmetic problem and outlined a comprehensive treatment plan.
Dr. Kapadia recommended a combination of lifestyle changes and medical treatments. Mrs Patel started wearing compression stockings, as advised and incorporated more leg exercises and elevation into her daily routine. She was amazed at how these simple changes brought significant relief.
However, to address the more severe symptoms, Dr. Kapadia performed a minimally invasive procedure to close off the problematic veins. The procedure was a success, with minimal discomfort and a quick recovery time.
Life After Treatment:
Post-treatment, Mrs. Patel experienced a remarkable improvement in her symptoms. The pain and swelling reduced drastically, and she was able to return to her active lifestyle. She felt a renewed sense of energy and was grateful for the effective treatment and care provided by Dr. Kapadia.
A Message of Awareness and Hope:
Mrs Patel’s story is a testament to the importance of not overlooking varicose veins as mere cosmetic issues. Her journey from pain and discomfort to relief and mobility is a message of awareness and hope for others experiencing similar symptoms.
Varicose veins, while common, should not be underestimated, especially when they cause pain and discomfort. With Dr. Sumit Kapadia’s expertise at Aadicura Superspeciality Hospital, effective treatment and management are within reach. For consultations, contact Dr Sumit Kapadia’s appointment number or send a “Hi” to +91 9904114443 on WhatsApp (Dr Sumit Kapadia’s 24 x 7 Vascular Helpline).

MBBS, MS, MRCS, DNB-Fellow
Dr. Sumit Kapadia
Dr. Sumit Kapadia / MR KAPADIA SUMIT a gold-medalist from Baroda Medical College, obtained his general surgical training and senior residency from SSG Hospital, Vadodara.

MBBS, MS, MRCS, DNB-Fellow
Dr. Sumit Kapadia
Dr. Sumit Kapadia / MR KAPADIA SUMIT a gold-medalist from Baroda Medical College, obtained his general surgical training and senior residency from SSG Hospital, Vadodara.



