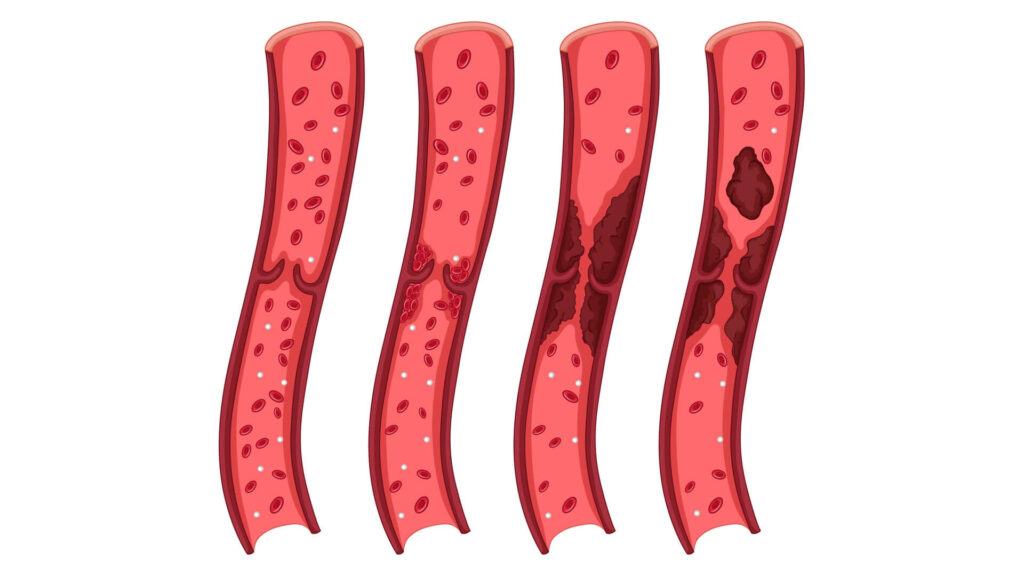
Peripheral Angioplasty is a life-enhancing medical procedure offered by Dr. Sumit Kapadia, a renowned specialist in vascular health. This treatment is essential for patients suffering from Peripheral Artery Disease (PAD), a common circulatory problem where narrowed arteries reduce blood flow to the limbs. PAD often leads to discomfort, and pain while walking, and can severely impact the quality of life. Through Peripheral Angioplasty, Dr. Kapadia aims to restore normal blood flow, alleviate pain, and prevent serious complications like leg ulcers or even amputation.
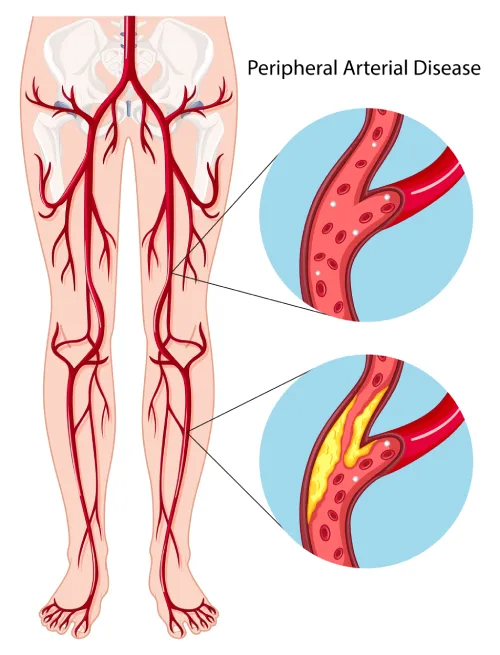
What the Treatment Involves
![]()
Benefits and Effectiveness
![]()
- Improving blood circulation in the legs.
- Reducing symptoms like pain and cramping during walking.
- Decreasing the risk of leg ulcers or, in severe cases, amputation.
Who Should Consider Peripheral Angioplasty?
![]()
- Cramping, tiredness, or pain in the legs or hips while walking or climbing stairs.
- Leg numbness, weakness, or heaviness.
- Coldness or colour change in the lower legs or feet
- Slow-healing sores on feet or legs.
- Change in the colour of the legs.
- Decreased nail and hair growth on the legs.
- Gangrene of toes
Before Your Angioplasty and Stenting Procedure
![]()
Preparing for the Procedure
Before undergoing peripheral angioplasty and stenting, Dr Sumit Kapadia and his team will guide you through a thorough preparation process to ensure the best outcomes:
Medical Evaluation: You’ll undergo a detailed medical evaluation, including blood tests, and possibly, an imaging test like an angiogram to assess the condition of your arteries.
Medication Review: Inform Dr. Kapadia about all the medications you are currently taking, including over-the-counter drugs and supplements. Certain medications might need to be adjusted or stopped before the procedure.
Fasting: You will likely be asked to fast for several hours before the procedure. This is standard practice for procedures performed under anaesthesia.
What to Bring: Wear comfortable clothes and bring any necessary personal items, as you might stay in the hospital for a short period after the procedure.
What to Expect During Peripheral Angioplasty and Stenting
![]()
During the Procedure
Understanding what happens during peripheral angioplasty and stenting can help alleviate any anxiety:
Anesthesia: The procedure is typically performed under local anesthesia, which means you’ll be awake but the area being worked on will be numb.
Catheter Insertion: A small incision is made, usually in the groin area, through which a catheter (a thin, flexible tube) is inserted. Using real-time X-ray images as a guide, the catheter is navigated to the blocked artery.
Angioplasty: Once the catheter reaches the blockage, a small balloon at its tip is inflated. This opens up the artery by pushing the plaque against the artery wall.
Stenting: In many cases, a stent (a small, metal mesh tube) is placed in the opened area to help keep the artery open.
Monitoring: Your vital signs will be closely monitored throughout the procedure. The entire process may take a few hours.
Completion: Once the procedure is completed, the catheter is removed, and pressure is given on the puncture site for 30 minutes. After this, we usually recommend to keep the leg straight for 6 to 8 hours.
Understanding these steps helps in preparing patients for what to expect during the angioplasty and stenting procedure, reducing apprehension and ensuring they are well-informed and comfortable with the process.
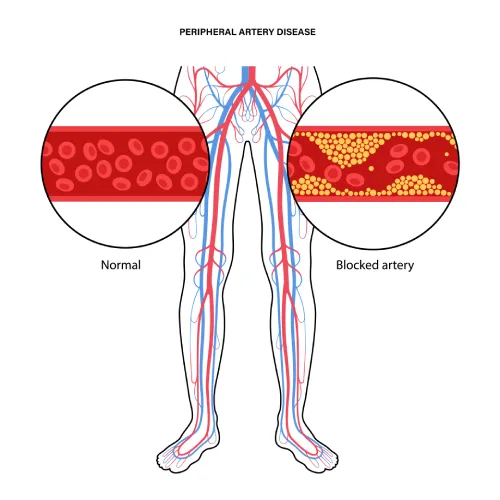
Recovery and Aftercare
![]()
Frequently asked questions
![]()
Peripheral Angioplasty is a procedure used to open up blocked or narrowed arteries in the legs. It is done to improve blood flow, relieve symptoms of PAD, and reduce the risk of leg ulcers or amputation.
The procedure typically takes between 1 to 2 hours. It is performed under local anaesthesia, so while patients may feel some pressure or mild discomfort, severe pain is uncommon. If patient has severe rest pain or painful ulcers, we may administer spinal or general anesthesia.
Most patients can go home on the same day or next day of the procedure. Recovery involves a brief period of rest, and most can return to normal activities within a week. It’s important to follow Dr. Kapadia’s advice on medication, lifestyle changes, and follow-up appointments for optimal recovery.
As with any medical procedure, there are some risks, but they are relatively low. These can include bleeding at the catheter insertion site, infection, artery damage, and rare cases of more serious complications. Dr. Kapadia’s expertise and the use of advanced techniques minimize these risks.
Post-procedure, maintaining a healthy lifestyle is crucial. This includes quitting smoking, controlling blood sugar if you’re diabetic, regular exercise, and a healthy diet. Regular check-ups and following medical advice are also essential for long-term health.
The two main types of angioplasty are balloon angioplasty, where a small balloon is inflated inside the artery to open the blockage, and stent angioplasty, where a stent (a tiny wire mesh tube) is placed in the artery to keep it open.
The success rate of peripheral angioplasty is high, typically over 90%. Success rates may vary depending on the severity of the blockage, the patient’s overall health as well as the location of the blockage ( below knee blockages have lower success rates)
In peripheral angioplasty, materials such as medical-grade plastic and metal (for stents) are used. The catheters and balloons are usually made of flexible, durable plastics, while stents are made of metal alloys.
The cost of peripheral angioplasty can vary widely based on the hospital, the complexity of the procedure, and whether stents are used. It’s best to consult with Dr. Sumit Kapadia for specific pricing information.
The risks of peripheral angioplasty include bleeding at the catheter insertion site, infection, damage to the blood vessel, and rare chances of more serious complications like a heart attack or stroke.
The procedure itself typically takes 1 to 2 hours, but this can vary depending on the complexity of the case.
Most patients can return home the same day and resume normal activities within a week. Full recovery and the realization of the procedure’s benefits may take a bit longer.
Peripheral angioplasty is done to restore blood flow in narrowed or blocked peripheral arteries, usually in the legs, to relieve symptoms of PAD and prevent complications like leg ulcers or amputation.
The best type of angioplasty depends on the patient’s specific condition. Dr. Kapadia evaluates each case to determine whether balloon angioplasty, stent angioplasty, or a combination of both is the most suitable.
Angioplasty is generally recommended when the arterial blockage is significant enough to cause symptoms or pose a risk for complications. Blockages over 70% are often treated with angioplasty.
Peripheral artery stents are designed to be permanent solutions. They typically last a lifetime, although patients need to manage their overall health to prevent new blockages from forming.
Testimonials
![]()
Peripheral Angioplasty Videos
![]()
Peripheral Angioplasty Related Blogs
![]()