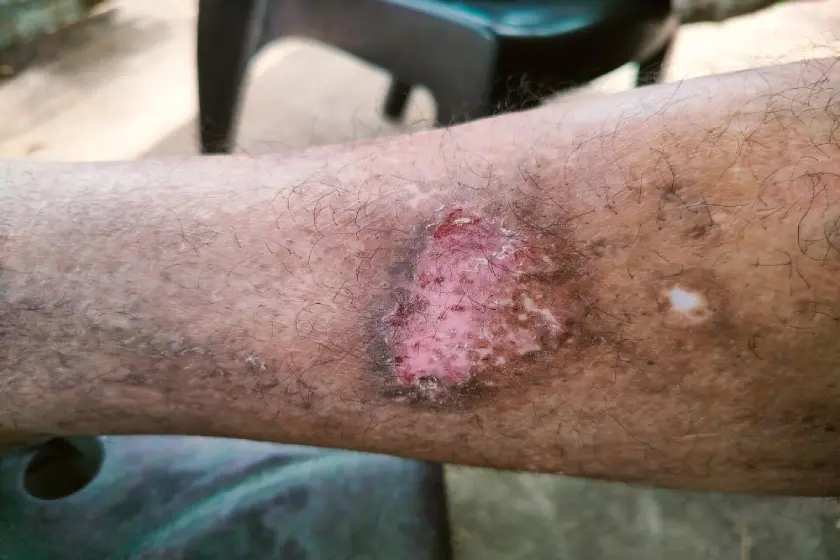
When you look at a wound on your leg that has refused to heal for weeks, you aren’t just looking at a skin problem: you are looking at a circulation system that has officially gone on strike. As a vascular specialist practicing here in Surat, I see patients every day who have tried every ointment and home remedy in the book, only to find that the small scratch on their ankle has turned into a stubborn, painful crater.
This is what we call a leg ulcer, and it is the ultimate red flag from your body telling you that your blood flow is in serious trouble.
In our busy city, where we spend hours standing at textile markets or sitting in offices, our legs take a massive beating, and often, we don’t realize the damage until the skin literally breaks open.
What Is a Leg Ulcer?
A leg ulcer is technically defined as a chronic wound that fails to heal within four to six weeks. While a normal cut or scrape heals because your body sends fresh blood and nutrients to the site, a leg ulcer persists because that delivery system is broken.
Think of your leg as a high-pressure plumbing system: when the pipes are clogged or the valves are leaking, fluid starts to seep into the surrounding tissue. This fluid buildup creates a toxic environment where the skin becomes thin, fragile, and eventually disintegrates into an open sore.
It is not just a sore that needs a bandage; it is a sign of underlying vascular failure that requires professional intervention.
Common Symptoms of a Leg Ulcer
The signs of an impending ulcer often show up long before the wound actually appears. You might notice a heavy, aching sensation in your calves that gets worse by the time you reach home in the evening.
This is usually accompanied by swelling around the ankles and a strange, leathery darkening of the skin known as hyperpigmentation. Once the ulcer starts to form, you will see a shallow red or yellow sore that might ooze clear fluid or pus.
The most telling leg ulcer symptoms are the persistent itchiness and the tight feeling of the skin around the wound, which indicates that the internal pressure is reaching a breaking point.
What Causes Leg Ulcers?
The primary culprit behind these non-healing wounds is almost always a breakdown in blood circulation. In most cases, the valves in your veins that are supposed to push blood back up to your heart stop working properly, causing blood to pool in your lower legs.
This increased pressure forces fluid into the skin tissue, causing it to break down from the inside out. Other leg ulcer causes include poor arterial supply, where not enough oxygen reaches the feet, or complications from long-term diabetes that damage the nerves and blood vessels simultaneously.
In a city like Surat, where lifestyle diseases are on the rise, these circulatory issues are becoming incredibly common among adults over forty.
Types of Leg Ulcers
Not all ulcers are created equal, and identifying the specific types of leg ulcers is the first step toward a successful cure.
Venous (Varicose Vein) Ulcers
These are the most common types I treat and are directly linked to varicose veins. They usually appear around the bony part of the ankle and are characterized by irregular edges and a purple or brown tint to the surrounding skin.
Diabetic Ulcers
These usually form on the bottom of the feet or over bony prominences. Because diabetes causes nerve damage, many patients don’t even feel the wound until it becomes a severe case requiring urgent leg wound treatment.
Arterial Ulcers
Unlike venous ulcers, these are caused by a lack of oxygenated blood reaching the leg. They are often very painful, look punched out and circular, and are usually located on the toes or heels.
Pressure Ulcers
Commonly known as bedsores, these occur when constant pressure on a specific area cuts off blood flow, typically in patients who are immobile for long periods.
Stages of a Leg Ulcer
Understanding the stages of a leg ulcer can help you realize the urgency of the situation. It begins with Stage One, where the skin is red and doesn’t turn white when pressed, indicating early tissue distress.
By Stage Two, the skin breaks, forming a shallow open sore.
Stage Three involves the wound deepening into the fat layer beneath the skin, and Stage Four is the most critical phase, where the ulcer reaches the muscle or bone.
At this final stage, the risk of systemic infection and even amputation becomes a very real concern, which is why early detection is vital.
How Are Leg Ulcers Diagnosed?
When you visit my clinic in Surat, we don’t just look at the wound; we look at the flow. Diagnosis usually involves a non-invasive Color Doppler Ultrasound to visualize the blood flow in your veins and arteries.
We also check your Ankle Brachial Index to compare the blood pressure in your arms and legs. These tests tell us exactly where the blockage or leakage is occurring, allowing us to create a roadmap for treatment rather than just guessing with different bandages.
Leg Ulcer Treatment Options
The goal of treatment is twofold: we must heal the open wound and fix the underlying circulation problem so it never comes back.
Medical & Wound Care Treatment
This involves specialized dressings that manage moisture and fight infection. We often use compression therapy, which involves high-grade bandages or stockings that manually push the stagnant blood back toward the heart, reducing the internal pressure that caused the ulcer in the first place.
Advanced Leg Wound Treatment
For stubborn cases, we utilize advanced leg wound treatment such as vacuum-assisted closure or skin grafting. However, the most modern approach involves treating the source of the problem through minimally invasive procedures that repair the damaged veins without the need for traditional surgery.
Varicose Vein Ulcer Treatment
If your ulcer is caused by varicose veins, simply dressing the wound is like mopping the floor while the tap is still running. For effective varicose vein ulcer treatment, we use advanced Laser or Radiofrequency Ablation to seal off the diseased veins.
This immediately diverts blood to healthier vessels, dropping the pressure in the leg and allowing the ulcer to heal at an accelerated pace.
Most patients are surprised to find that a procedure taking less than an hour can solve a wound they have been struggling with for months.
When Should You See a Leg Ulcer Doctor?
You should never wait for a wound to see if it heals on its own.
If you notice a sore that hasn’t improved in two weeks, if the wound smells foul, if you have a fever, or if the skin around the sore is becoming red and hot to the touch, you need to see a leg ulcer doctor immediately.
These are signs of a spreading infection that can quickly lead to cellulitis or sepsis.
Why Consult a Vein Specialist Doctor in Surat?
Surat has some of the best medical infrastructure in Gujarat, and as a vein specialist doctor in Surat, I have access to the latest laser technology and diagnostic tools.
Seeing a vascular specialist ensures that you aren’t just getting a temporary fix from a general practitioner but are addressing the biological root cause of your leg pain and wounds.
We focus on long-term limb salvage and ensuring that you can get back to your daily work without the fear of recurring sores.
Conclusion
A leg ulcer is a serious medical condition, but with the right vascular care, it is entirely treatable. You don’t have to live with the pain, the bandages, and the constant worry about infection.
By addressing the circulation issues early, we can close the wound and restore the health of your legs.
If you or a loved one is struggling with a non-healing leg wound, take the first step toward recovery today: stop focusing on the skin and start focusing on the flow.
Frequently Asked Questions
The best leg ulcer treatment is a combination of specialized wound dressings and addressing the underlying vascular cause, such as using laser treatment for varicose veins or compression therapy for venous insufficiency.
The final stage is Stage Four, where the ulcer penetrates deep into the muscle, tendons, or even the bone, posing a high risk of severe infection and bone damage.
It usually starts as a patch of discolored, reddish, or dark brown skin that feels itchy, hard, or warm to the touch before the skin actually breaks.
Avoid high-sodium foods, which increase swelling, sugary snacks that impair healing, and processed fats that can worsen arterial blockages.
Focus on protein-rich foods like lentils and eggs to repair tissue, Vitamin C sources like amla and citrus fruits to boost collagen, and Zinc-rich seeds to accelerate the closing of the wound.

Dr. Sumit Kapadia
MBBS, MS, MRCS, DNB-Fellow



